Ichthyosis
General Information
Ichthyosis is not one disease but a group of disorders in which there is excess accumulation of epidermal cells resulting in the appearance of scales. The ranges of severity go from mild, asymptomatic, to life threatening. There are different types of ichthyosis; most are extremely rare. The condition worsens in the dry, cold winter months and generally improves in the warmer, more humid months of summer. The most common type of ichthyosis is ichthyosis vulgaris, which accounts for almost 95% of cases. Ichthyosis vulgaris affects about 1:250 individuals. The signs and symptoms vary among the different types of ichthyosis, but they all show the same characteristics of dry, rough, scaly skin. Treatment is mainly focused on moisturizing and exfoliating these rough patches. Creams and ointments to keep the condition under control may be prescribed. In more severe cases, a health care provider may prescribe oral retinoids such as acitretin or isotretinoin. If a secondary infection occurs, oral antibiotics may be prescribed. People with ichthyosis have normal lifespan although they may need to spend several hours each day caring for their skin.
Epidemiology
Relatively uncommon group of skin disorders
Etiology
Genetic defect (either by spontaneous mutation of a gene or through family inheritance
Pathogenesis
Excess accumulation of epidermal cells resulting in the appearance of scales
Clinical
Dry, rough, scaly skin
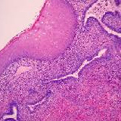
Histology
Ichthyosis vulgaris – Mild hyperkeratosis and diminished granular layer in the epidermis. Xlinked ichthyosis – Expanded stratum corneum without parakeratosis or acanthosis. Lamellar ichthyosis – Massive, compact orthohyperkeratosis with variable degrees of parakeratosis and markedly thick stratum corneum. Epidermolytic hyperkeratosis – Epidermal acanthosis and hyperkeratosis.
Bibliography
1. “Ichthyosis” (Online). http://www.aocd.org/skin/dermatologic_diseases/ichthyosis.html (visited: March 19, 2008) 2. “Ichthyosis” (Online). December 2007. http://www.emedicine.com/oph/topic687.htm (visited: March 19, 2008)
Download PDF
![]() Ichthyosis
Ichthyosis