Tinea
General Information
Tinea is a fungal infection that occurs on the surface of the skin. The agents that cause the fungus are dermatophytes (means skin fungi), which invade the dead keratin of the skin, hair and nails. Humidity and moisture provides a favorable environment for the establishment of fungal infections. Clinically, tinea infections are classified by the region on the body involved. Tinea Capitis – Infection of the scalp hair; clinical varies depending on the hair invasion, hair breakage and loss of hair may occur. Tinea Corporis – Infection of the trunk and extremities; characterized by annular, scaly plaques, pustules and vesicles. Tinea Cruris – Infection of the groin and pubic region; erythematous lesions. Tinea Pedis – Infection in the web of the toes and plantar surface; characterized by toe-web scaling, fissuring, and macerations, vesicles, pustules, and bullae. Tinea Unguium – Infection of the nail; characterized by thickened, discolored, and broken nails. Common causes exists for all different types of tinea including, moist conditions, communal showers and athletic activities. Tinea can be treated topically with antifungal creams that contain clotrimazole, lotrimin, miconazole, ketoconazole, and terbinafine. Tinea can also be treated with systemic medications, which include terbinafine, itraconazole, and fluconazole.
Epidemiology
Fungal infections occur worldwide. Tinea Pedis is the most common in the United States
Etiology
Caused by species of the genera Microsporum, Trichophyton, and Epidermophyton
Pathogenesis
Inflammatory process caused by superficial fungi
Clinical
Tinea Capitis – Thickened, scaly, swellings, or as expanding raised red rings with central healing, Tinea Corporis – Enlarging raised red rings with a central area of healing, Tinea Cruris – Red, tan, or brown, with flaking, peeling, or cracking skin, Tinea Pedis – Scaling, flaking blisters and cracked skin, Tinea Unguium – Nail plate is thickened, yellow, or cloudy, Tinea Versicolor – Oval or irregularly-shaped spots of 1/4 to 1 inch in diameter.
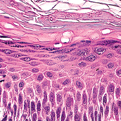
Histology
Hyperkeratosis with variable neutrophil infiltrates and spongiosis. The dermis may have a mixed inflammatory infiltrate and tinea can cause subepidermal bulla formation (Easily demonstrated with PAS (periodic acid Schiff) stains that stain fungal hyphae walls).
Bibliography
1. “Tinea” (Online). November 2006. http://www.emedicine.com/EMERG/topic592.htm (visited: April 4, 2008) 2. “Ringworm (Tinea)” (Online). November 2007. http://www.medicinenet.com/ringworm/article.htm (visited: April 4, 2008)
Download PDF
![]() Tinea
Tinea